
A guide for treating MARCoNS – a nasal staph infection
MARCoNS: Just a glance at the acronym looks like trouble. MARCoNS stands for multiple-antibiotic resistant coagulase-negative Staphylococci — which means it’s an antibiotic-resistant staph bacteria, one that resides deep in the nasal passages. In other words, it’s a nasal staph infection.
Technically, it’s not an infection but a commensal bacterial colonization that can become a nasal staph infection, like other potentially pathogenic bacteria that coexist in the human body. Commensal bacteria are normal flora consisting of microorganisms, which can inhabit our gastrointestinal/respiratory tracts, vagina, skin, and other areas.
MARCoNS is considered a controversial condition in some circles as a segment of the medical community claims it’s not recognized by medical science as a “real” diagnosis.
Nevertheless, coagulase-negative Staphylococci (CoNS) are routinely found in healthy people, particularly on the skin.1 Problems can arise when certain strains of potentially pathogenic bacteria proliferate and create an imbalance in the body.
MARCoNS is difficult to treat, yet patients have resolved this complicated infection by employing a combination of treatment strategies (including patience), which we’ll explore in this article.
Before you treat, find out the root cause of MARCoNS
MARCoNS is not commonly found deep in the sinuses of individuals with normal, intact immune systems. It’s more common in patients who have mold exposure with the accompanying mycotoxins (toxic compounds given off by certain types of mold).2
In addition to mold exposure, MARCoNS is common in patients with autoimmune conditions and biotoxin-related illnesses, like chronic fatigue syndrome (CFS), chronic fatigue, immune dysfunction syndrome (CFIDS), chronic Lyme disease, and chronic inflammatory response syndrome (CIRS).3
Symptoms of CIRS appear similar to what one would expect to see in patients dealing with an infection in the nasal passages, indicating that there could be a link between MARCoNS and CIRS.

Pathogenic coagulase-negative Staphylococci bacteria can interfere with multiple functions in the body.4 For example, it releases exotoxins A and B (bacterial toxins that inhibit cell function) into the bloodstream. These chemicals, manufactured by harmful bacteria, exist in the nasal passages but cause systemic damage through increasing inflammatory responses.5
Staph coagulase-negative bacteria can become resistant to multiple antibiotics (hence, the term MARCoNS) due to a protective substance known as a biofilm. Biofilms encase the bacteria — as if they were walled off in a fortress — and block antibiotics from entering.6 Biofilms make chronic infections much more difficult to treat.
Supplementing with EDTA (a substance that can grab and bind to other molecules, acting as a detoxifying agent) and N-Acetylcysteine (NAC) may help break apart biofilm, allowing antibiotics, antifungals, and other treatments to reach and destroy pathogens.2
What MSH (melanocyte-stimulating hormone) has to do with MARCoNS
Melanocyte-stimulating hormone (MSH) is one of a number of hormones that the pituitary gland, hypothalamus, and skin cells produce. It’s a powerful anti-inflammatory and helps to regulate inflammatory responses, so it’s vitally important to keep MSH levels in balance.7
This is because:
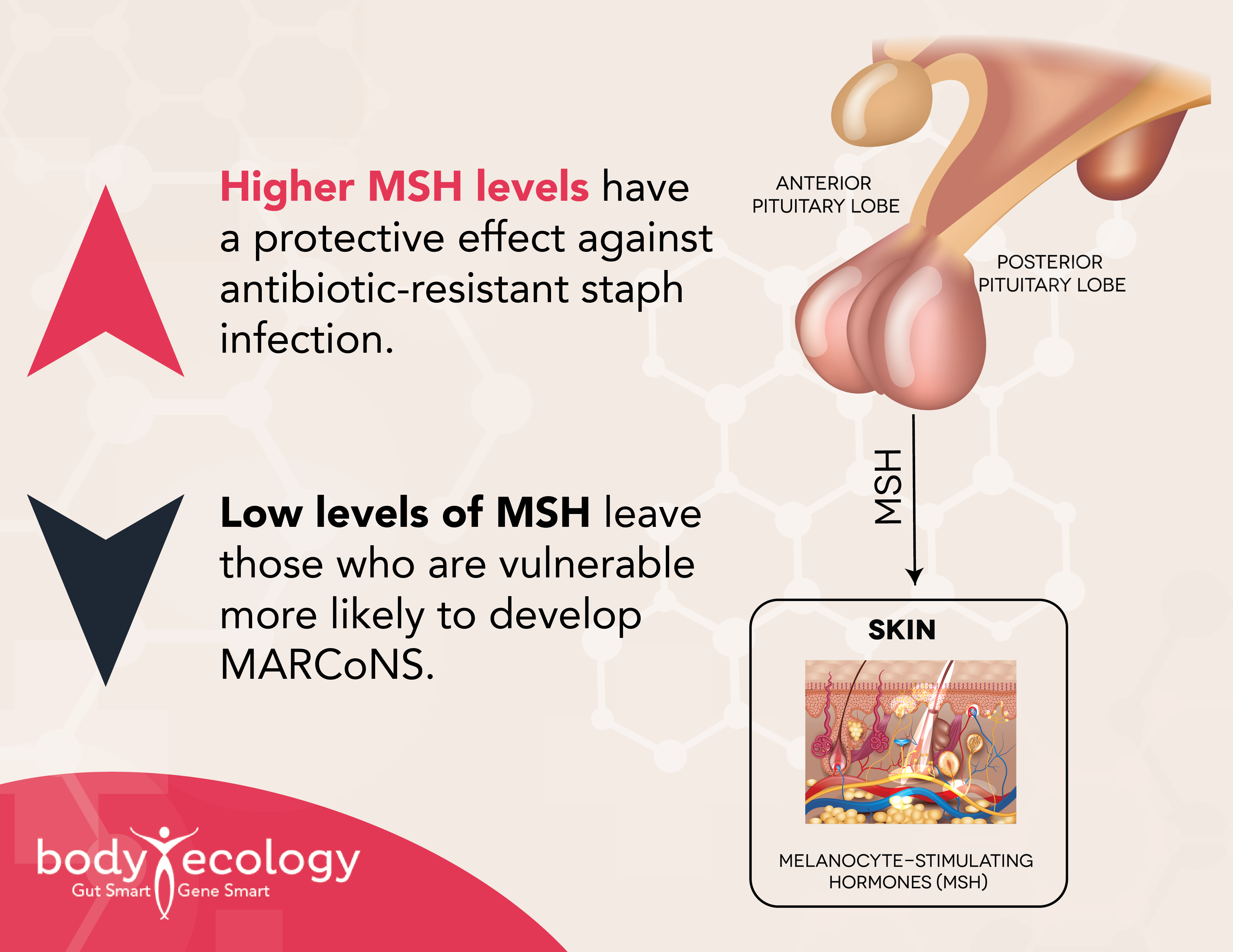
Low MSH is caused by increased inflammation, triggered by cytokines reacting to biotoxins (mold and Lyme) in the body. Those that suffer from biotoxin illnesses, such as chronic Lyme disease and mold exposure, are more prone to these inflammatory conditions that lower MSH.
Complicating matters, people with CIRS often have low levels of MSH, making them even more susceptible to MARCoNS. Eighty percent of those with low MSH are thought to have MARCoNS.8 Furthermore, the incidence of patients with low MSH also having MARCoNS increases if the patient has been taking antibiotics for a month or longer.9
As MARCoNS-associated MSH levels decline further, fatigue and chronic pain become an issue — as a result of diminished endorphin release and increased cytokine activity. Low levels of MSH may also be responsible for hormonal imbalances, mood swings, leaky gut, problems with proper bowel elimination, and low melatonin (leading to sleep disruption).10
When MSH falls too low, the body will respond by raising Adrenocorticotropic Hormone (ACTH). In times of stress, ACTH contributes to a surge in cortisol.11 This activity serves to keep the body functional in the face of the increased stress.
Eventually, the body can’t keep up. ACTH and cortisol levels can drop low enough to create compromised adrenal function.
In short, reduced MSH can be considered a cofactor that could disrupt multiple biological processes, which contribute to MARCoNS taking hold as a nasal staph infection. Genetic testing (known as HLA-DR) is available and can be used to determine if there’s an immune deficiency present that prevents the body from being able to excrete Lyme, bacterial, or mold toxins.
Let’s get better together. Listen and subscribe to the Body Ecology Living Podcast.
How to raise MSH and eradicate MARCoNS
There are strategies available that can help increase MSH levels by destroying biotoxins, leading to the eventual elimination of MARCoNS:
- Removing the patient from the source of toxicity is the first step toward healing and contributes to ultimately raising MSH back to healthy levels. A moldy home, office, or other location the patient visits frequently is usually the source of initial exposure. Remediation of the building, or even moving to a new home, if possible, should be realized as soon as possible to avoid continual reexposure.
- When the immune system is compromised, it’s always crucial to support gut health. Seventy percent of the immune system resides in the gut.12 A diverse, healthy microbiome, teeming with beneficial bacteria, and a tight gut lining are foundational to achieving good gut health — and good health overall.
Whether you’re supporting your gut with multiple strains of beneficial bacteria and providing a source of nourishment for those bacteria, and/or consuming foods and beverages that contain healthy microbes that will colonize in the gut, Body Ecology offers a complete selection of delicious foods, beverages, and probiotics that provide benefits to support MARCoNS treatment options.
In addition to sustaining the gut with effective lifestyle and nutritional interventions, Vasoactive Intestinal Polypeptide (VIP), a gut-peptide hormone nasal spray with a variety of functions, may help correct neuroendocrine abnormalities that in turn regulate nutrient absorption, motility, blood sugar control, immune system responses, and circadian rhythms.
Improvements in neuroimmune response resulting from VIP neuropeptide treatment have also shown benefit related to many physiological functions involved in gastrointestinal function — which includes increasing MSH levels, known to improve both chronic fatigue symptoms and MARCoNS.13
In short, VIP is a hormone treatment that helps support healthy levels of other hormones. It’s often considered the last strategy in the healing journey for CIRS patients once gut health is addressed, and other protocols are implemented. It’s available only by prescription from a compounding pharmacy.
Again, supporting the immune system systemically by bolstering gut health is vital. In addition, using a nebulizer and doing nasal rinses are effective in fighting nasal pathogens and MARCoNS. Healthcare practitioners are recommending that their patients use certain natural antibacterials in a nebulizer (or nasal rinse) twice a day.
Natural choices could include Biocidin, colloidal silver, and propolis. (Or all three together.) Xylitol in the water breaks up biofilms. Hydrogen peroxide is especially effective but may be too harsh for some. Try nebulizing a diluted solution of hydrogen peroxide with water (1 quart water to 1 tablespoon hydrogen peroxide). Quinton minerals prove helpful as well.
Healing from biotoxin illnesses can be a long journey. But functional medicine recommendations and interventions exist, and more are being developed that are making recovering from chronic illness possible.
REFERENCES:
- 1. Becker K, Heilmann C, Peters G. Coagulase-negative staphylococci. Clin Microbiol Rev. 2014;27(4):870-926. doi:10.1128/CMR.00109-13.
- 2. Forsgren, Scott. “Mold and Mycotoxins: Often Overlooked Factors in Chronic Lyme Disease.” Townsend Letter, 2014.
- 3. “Chronic Inflammatory Response Syndrome (CIRS).” Parliament of Australia, 2018.
- 4. Philip Toltzis, 116 – Staphylococcus epidermidis and Other Coagulase-Negative Staphylococci, Editor(s): Sarah S. Long, Charles G. Prober, Marc Fischer, Principles and Practice of Pediatric Infectious Diseases (Fifth Edition), Elsevier, 2018, Pages 706-712.e4, ISBN 9780323401814, https://doi.org/10.1016/B978-0-323-40181-4.00116-X.
- 5. T. Barbieri, Exotoxins, Editor(s): Moselio Schaechter, Encyclopedia of Microbiology (Third Edition), Academic Press, 2009, Pages 355-364, ISBN 9780123739445, https://doi.org/10.1016/B978-012373944-5.00225-X.
- 6. John JF, Harvin AM. History and evolution of antibiotic resistance in coagulase-negative staphylococci: Susceptibility profiles of new anti-staphylococcal agents. Ther Clin Risk Manag. 2007;3(6):1143-1152.
- 7. Singh M, Mukhopadhyay K. Alpha-melanocyte stimulating hormone: an emerging anti-inflammatory antimicrobial peptide. Biomed Res Int. 2014;2014:874610. doi: 10.1155/2014/874610. Epub 2014 Jul 23. PMID: 25140322; PMCID: PMC4130143.
- 8. “Inquiry into Biotoxin-related Illnesses in Australia, Submission 129.” Australian Chronic Infectious & Inflammatory Disease Society, 2018.
- 9. “MARCoNS – An Overview.” Microbiology DX, 2021.
- 10. Natasha Thomas, M.D. “Understanding Chronic Inflammatory Response Syndrome (CIRS).” 2016.
- 11. Allen MJ, Sharma S. Physiology, Adrenocorticotropic Hormone (ACTH) [Updated 2021 Aug 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan.
- 12. Vighi G, Marcucci F, Sensi L, Di Cara G, Frati F. Allergy and the gastrointestinal system. Clin Exp Immunol. 2008;153 Suppl 1(Suppl 1):3-6. doi:10.1111/j.1365-2249.2008.03713.x.
- 13. Aresti Sanz J, El Aidy S. Microbiota and gut neuropeptides: a dual action of antimicrobial activity and neuroimmune response. Psychopharmacology (Berl). 2019;236(5):1597-1609. doi:10.1007/s00213-019-05224-0.









