The Appendix: Not a Useless Organ
Chances are, you or someone you know has been rushed to the hospital with acute appendicitis. Out of seemingly nowhere, abdominal pain raced in with nausea and vomiting. Then came a fever and pronounced abdominal swelling. Something was wrong…and you ended up in the emergency room.
The attending ER physician diagnosed appendicitis and ordered an immediate appendectomy…before this (“accessory”) organ could burst, releasing large amounts of toxins into your body that could kill you.
While being prepped for surgery, the doctor assures you that the appendix is something the body can do without, that it really doesn’t perform a specific function, and “we” don’t really know why we have an appendix, anyway. But an inflamed organ filled with toxins, particularly one we can live without, must come out.

For decades, this was our understanding of and our medical approach to an appendix gone bad. But recently, new research shows our understanding of it has changed.
Humans Don’t Need an Appendix…?
The appendix is a small tube-like structure that connects to the colon at the point where the small intestine connects to the first part of the colon called the cecum. It resembles a pouch located right where the large intestine begins. The small intestine empties into the cecum. The size of your appendix is correlated with the size of your cecum and colon.
With its pouch-like shape it’s apparent that the appendix can’t move food and/or waste through the GI tract. Yet this so-called unnecessary “vestige” organ plays a role in the digestive process.
Many people have their appendix removed and do not appear to suffer any harm. This is likely the reason medical science believed the appendix to be merely an evolutionary holdover from millions of years ago. (Other animals also seem to have similar non-functioning structures.)
Now it seems, medicine is taking a different view.
How the Appendix Functions
The structure of the appendix suggests that it has a role in the movement and removal of waste in our digestive system. But there is a lot more to it.
This is what researchers at Duke University discovered and published in the Journal of Theoretical Biology in 2007: Good microbes may be eliminated from the body as a result of diseases such as dysentery or cholera, truly upsetting the digestive system (and very dangerous to boot.) The appendix comes to the rescue during these times and releases its store of good bacteria to “reboot” the digestive system.
According to Dr. William Parker, with the Duke University study, and lead researcher responsible for the theory of the appendix being a functional organ said, “the fact that the appendix is located at the lower part of the large intestine through which food and microbes pass, supports the theory that the appendix has some function related to the microbial flora of the digestive system.”
The Evolutionary Model
In another study from 2009, University of Arizona researchers examined the cecum appendix of multiple mammalian species over millennia. They studied their structure, function and genetic composition and compared them to the human appendix.
They concluded that an evolution in scientific thought and understanding related to gut immunity had emerged, one that deepened their knowledge of the symbiotic relationship between beneficial and pathogenic bacteria in the human gastrointestinal tract whereby the appendix evolved as a repository for beneficial gut microbes, preserving the microbiome during periods in evolutionary history when intestinal infection was rampant and so-called modern medicine hadn’t yet developed.
They went on to report that through their analysis of the data, they discovered the appendix has evolved in multiple mammalian species and has “been maintained in mammalian evolution for 80 million years or longer.”
Clearly, such diversity of bacterial species is critical to gastrointestinal health as the human appendix prioritized this important function over thousands of years.
The Protector
According to a 2011 study published in the journal Clinical Gastroenterology and Hepatology, the appendix appears to offer protection against Clostridium Difficile (C. diff) infection, a potentially dangerous bacteria causing diarrhea and an inflamed colon. C.diff infections have been on the rise in recent years.
In the 2011 study, researchers recruited people without an appendix and found they experienced recurrent C. diff. infections (CDI) in the intestines at a rate 2.5 times higher than those with an appendix. The study’s lead researcher Dr. J. H. Grendell reported, “the rate of CDI recurrence in patients with an appendix was 18%, compared with 45% in those without an appendix.”
They also found significant amounts of lymphatic follicles in the appendix, much like that which exists in other areas of the intestines. (Lymphatic follicle–a component of lymphatic tissue–is part of the lymphatic system). This type of lymphatic tissue is known as gut-associated lymphoid tissue (GALT.) GALT tissue performs important biochemical processes throughout the immune system.
When you hear someone say that the immune system is in the gut GALT that’s because it provides the greatest area of lymphoid tissue in the body and because:
- it contains B and T immune cells (lymphocytes), macrophages, and antigen-generating cells
- and epithelial and intra-epithelial lymphocytes which make up the gut lining.
These serve as the body’s first defense against infectious invaders protecting us against countless numbers of unseen, pathogenic invaders.
These, as well as other structures and functions of the appendix, indicate the appendix provides early protection that can prevent serious infections from taking hold in the body by keeping pathogens from proliferating, while allowing good microbes to thrive in the gut.
The appendix performs other important functions as well. Immune tissue in the appendix also has a high concentration of immunoglobulin, an even higher concentration (of IgA and IgG producing immunocytes) than does the colon, demonstrating the appendix must play an important role in fighting infection in the gut and preserving the mucosal lining.
The appendix also has an “appendiceal” biofilm, more proof that our appendix does indeed have a beneficial effect for the entire gut. Biofilms aren’t bad. Sure, they’re a problem when they house pathogens. But beneficial microbes form biofilms for protection as well. If commensal and beneficial bacteria are living in an appendiceal biofilm, the colon can be reseeded when these microbes are wiped out, for example with diarrhea.
Pathogenic bacteria can damage healthy tissue causing infection and disease and must be kept in check. Looking more closely at the natural balance between beneficial and pathogenic bacteria in the gut, beneficial bacteria do no harm to the colon as long as they stay in a beneficial or commensal form. In fact, they contribute to optimal health and immune function by keeping the overall gut bacteria in balance, crowding out dangerous pathogens, and making it difficult for those species to multiply.
What disrupts this natural balance? When the environment of the gut becomes toxic, even the commensals can change into a pathogenic form. Prescription antibiotics kill all bacteria, not just the bacteria causing the problem. This can allow pathogenic bacteria to get a stronghold in the gut, upsetting the natural microbial balance and leading to overgrowth of unwanted bacterial strains.
The CDC in fact, attributes the rise in C.diff infections to over-prescribing broad-spectrum antibiotics in seniors, making C. difficile bacteria more resistant to other antibiotics when they are really needed.
Note: Fermented vegetables and probiotic liquids should be taken when antibiotics are used. Yes, at the same time.
The Microbiome’s Safe House
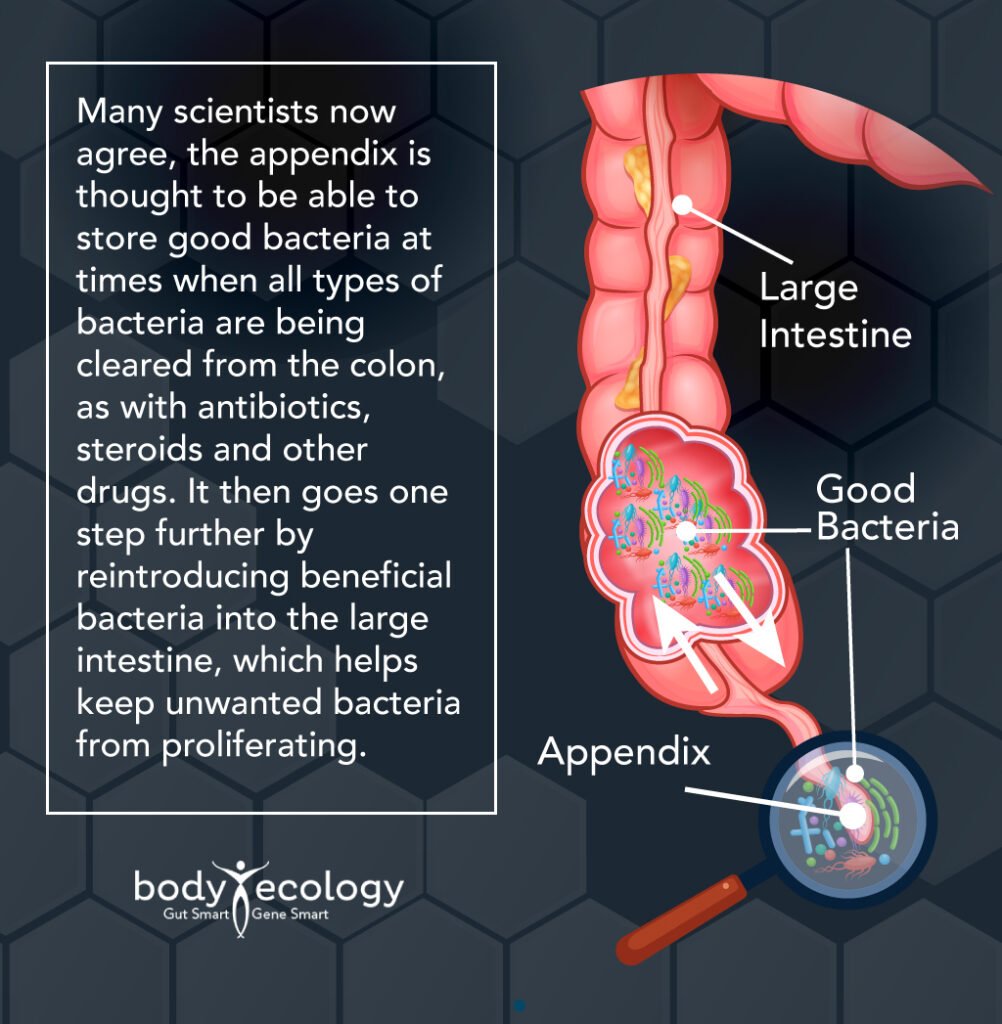
Many scientists now agree, the appendix is thought to be able to store good bacteria at times when all types of bacteria are being cleared from the colon, as with antibiotics, steroids and other drugs. It then goes one step further by reintroducing beneficial bacteria into the large intestine, which helps keep unwanted bacteria from proliferating.
When the alarming symptoms described earlier begin, it is usually due to a blockage in the lining of the appendix. This likely causes an infection that results in appendicitis. Bacteria can multiply quickly causing the appendix to become swollen, inflamed, and filled with pus. This is an emergency which must be dealt with immediately before the appendix can rupture. So please, don’t wait until this happens.
A good way to maintain the critical microbial balance is to follow The Body Ecology Way and a probiotic-rich diet, which protects and support balance in our gut.
We have Probiotic Liquids, cultured veggies, probiotics, GI Distress Relief. and even a phage called EcoPhage Microbiome Support.
In one study 85% of the 117 participants were infected with pathogenic E.coli as the main pathogen. EcoPhage selectively targets specific, harmful E. coli bacteria while leaving beneficial microbes to flourish.
85% of the 117 participants were infected with pathogenic E.coli as the main pathogen. EcoPhage selectively targets specific, harmful E. coli bacteria while leaving beneficial microbes to flourish.
Since pathogens form biofilms in the appendix EcoOxy-Zyme can be taken to help remove pathogenic biofilms.
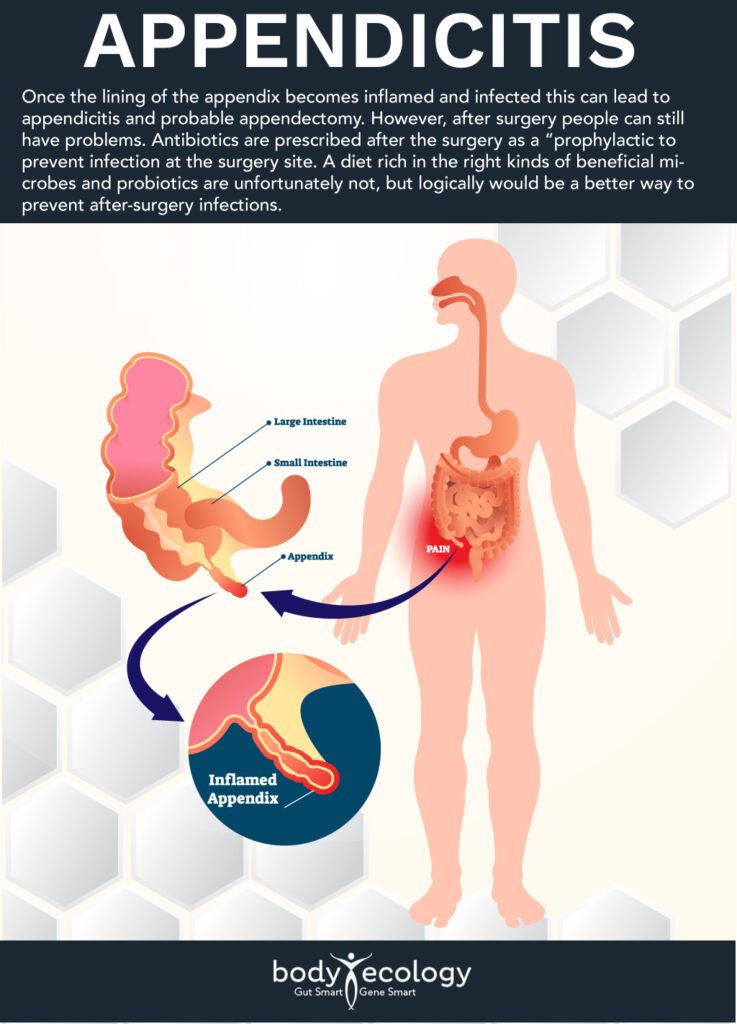
Like any organ or body system, the appendix can be susceptible to disease and dysfunction. As described above, once the lining of the appendix becomes inflamed and infected this can lead to appendicitis and probable appendectomy. However, after surgery people can still have problems. Antibiotics are prescribed after the surgery as a “prophylactic” to prevent infection at the surgery site. A diet rich in the right kinds of beneficial microbes and probiotics are unfortunately not, but logically would be a better way to prevent after-surgery infections.
Note: While unusual, cancer of the appendix does occur and is usually discovered when tissue removed during an appendectomy is analyzed during a routine biopsy and is found to contain carcinoid cells or tissue. Treatment usually involves surgery and removal of a section of the colon, sometimes followed by chemotherapy.









